Myeloma
Learn about myeloma
Myeloma is a bone marrow cancer. It is often called multiple myeloma, due to the multiple places in the body that bone marrow is found (e.g. in the spine, skull, shoulders, ribs and pelvis). When myeloma cells are only found in one part of the body, this is called plasmacytoma.
At ACRF we are committed to outsmarting cancers like Myeloma by improving prevention, diagnosis and treatment. According to Australian government statistics, Myeloma is the 17th most commonly diagnosed cancer in Australia and has a 51% chance of surviving at least 5 years.
The cause of Myeloma is unknown and is not considered hereditary. An increased risk of developing Myeloma is due to exposure to certain toxic chemicals, radiation immune disorders and viruses.
Myeloma arises in our plasma cells, which are mature white blood cells and form part of our immune system. When the myeloma cells start to abnormally reproduce, they form tumours that accumulate in the bone marrow or on the surface of different bones throughout the body. These tumours secrete chemicals that stimulate other bone marrow cells to remove calcium from the bone – resulting in weaker, more brittle bones.
Causes of myeloma remain largely unknown, but it is thought to result from damage to one or more of the genes that normally regulate blood cell development. Some people with a non-malignant condition called monoclonal gammopathy of undetermined significance (MGUS) will eventually go on to develop myeloma.
Myeloma cells also produce an abnormal antibody called paraprotein (also referred to as M-protein or monoclonal protein). Myeloma is often classified according to the type of paraprotein produced by the myeloma cell. This is often diagnosed or measured through the blood or the urine. Excessive amounts of paraprotein in the body can cause problems, such as kidney damage.
Most symptoms relating to Myeloma are caused by the build-up of abnormal plasma cells in the bone marrow (and the consequent disruption to abnormal blood cell production). They include:
- Bone pain, bone fractures or brittleness
- Tiredness
- Frequent or recurrent infections
The initial testing to detect and diagnose Myeloma includes blood and urine tests. Blood tests are used to determine the amount of Paraprotein that myeloma cells produce while urine tests for the presence of Bence Jones protein. Each of these shows an abnormality.
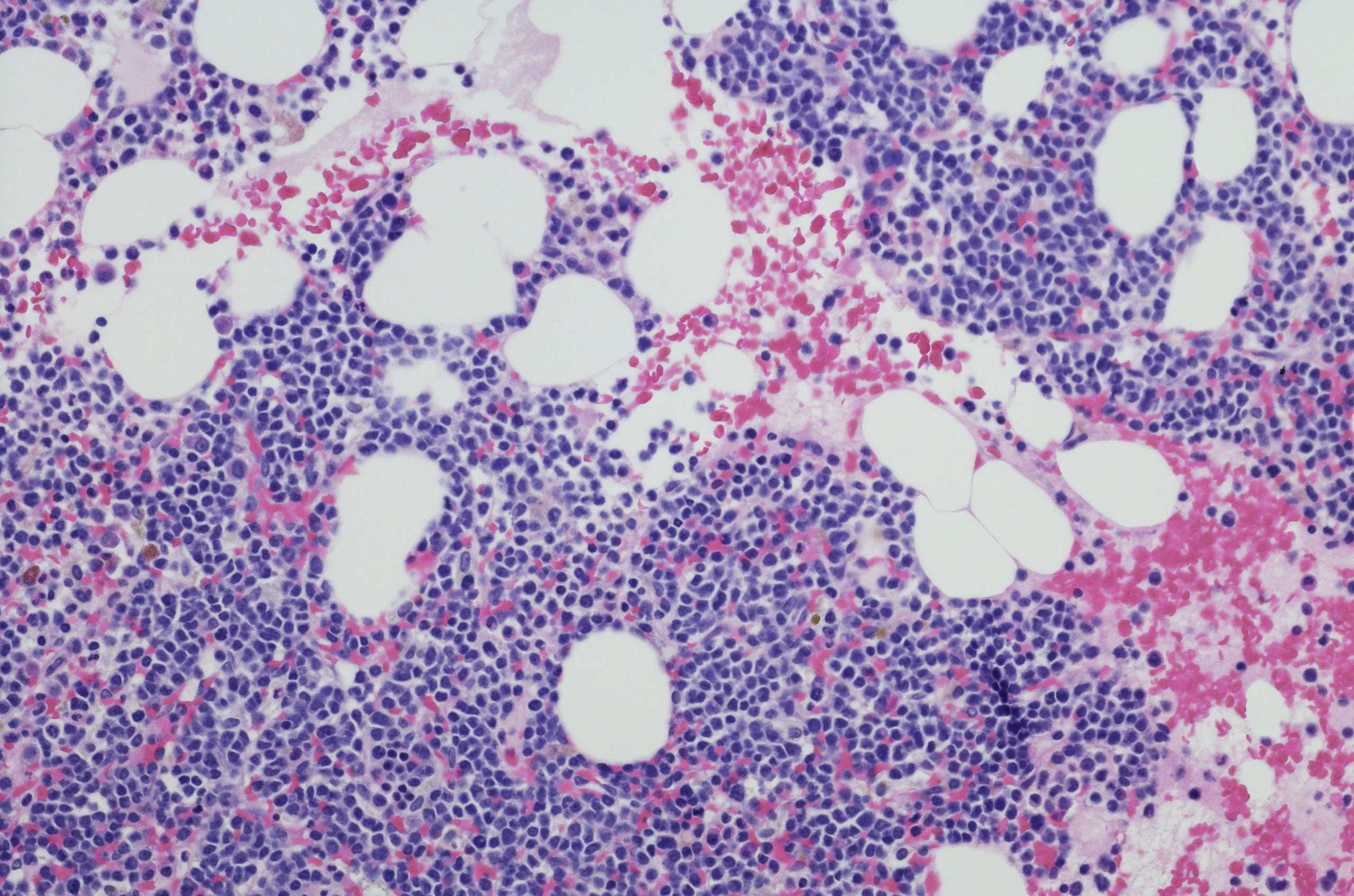
Another detection method is a bone marrow biopsy which is used to examine the cells from the marrow.
Other detection methods include X-rays, magnetic resonance imaging (MRI), computed tomography (CT) Scans and positron-emission tomography (PET) scans.
Current treatments for Myeloma are very effective at halting the disease’s progress and managing symptoms. Quality of life is improved, but the disease is not cured and regular monitoring is required.
Myeloma Diagnosis
While myeloma is typically detected through blood and urine tests, x-rays or scans of the bones might also be performed to determine if there are any weaknesses in the bone, or erosion from the myeloma cells. A bone marrow biopsy (which will take a small sample of bone marrow for examination) is also often required.
Myeloma Treatment
Specific treatment schedules will depend on the stage of the disease, the severity of symptoms and the patient’s general health. Even if the disease has been diagnosed in its early stages, usually there are no symptoms and so treatment is not required immediately. It can be months or years before symptoms show themselves. In these cases, the treating doctor will recommend regular check-ups, including blood and urine tests.
To control the growth of myeloma, chemotherapy is often used in combination with cortico-steroids. This treatment will continue until the myeloma reaches a stable stage (where the amount of myeloma cells is reduced to as low as possible). Treatment to prolong remission will then be advised.
Patients may also require treatment to treat any bone damage from the myeloma. A family of drugs called bisphosphonates may be used to re-strengthen the bone and reduce any risk of fractures. These therapies also have the effect of minimising bone pain and excess calcium in the blood.
On occasion, a stem cell transplant will be advised by your doctor.