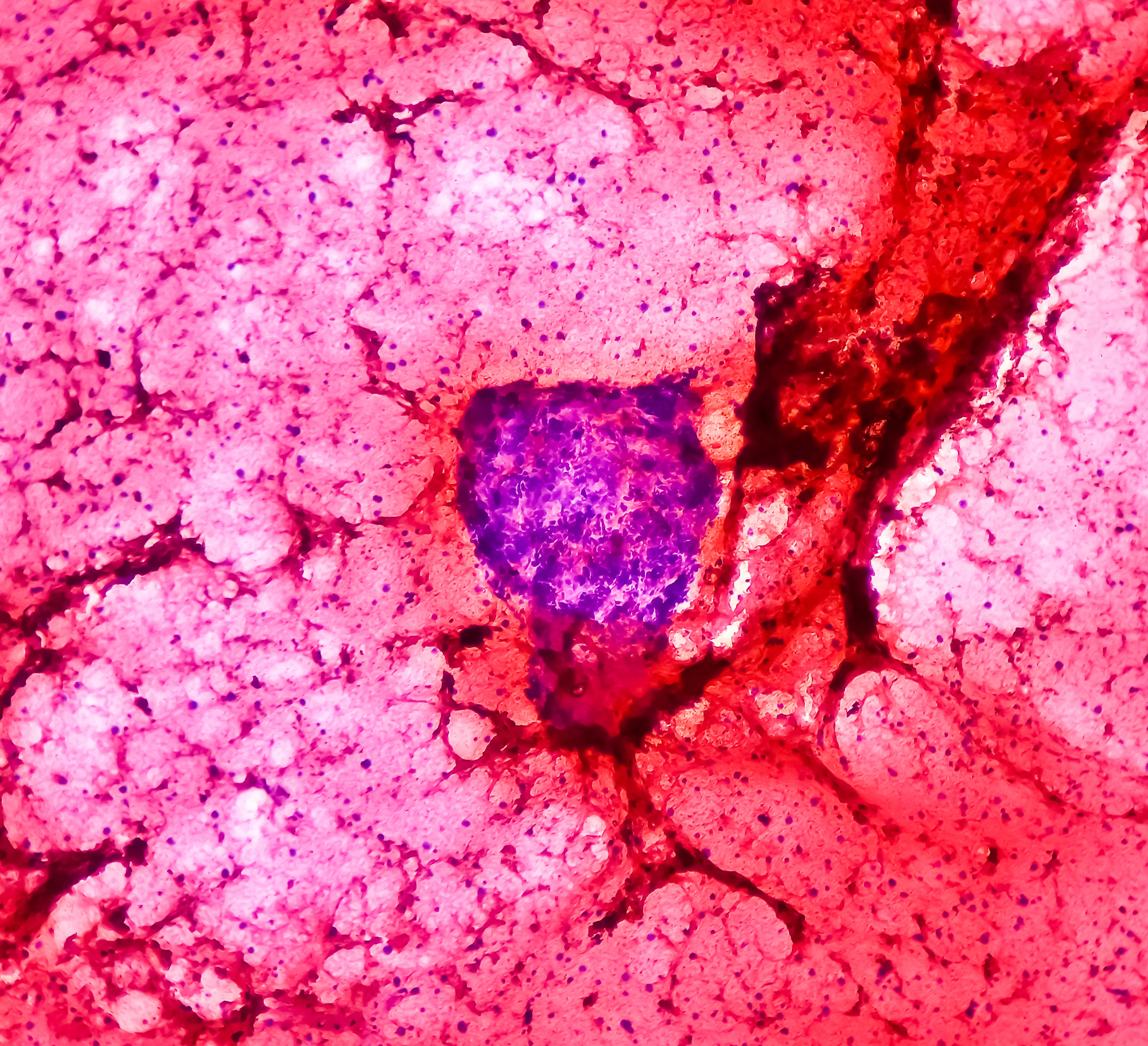
Ewing Sarcoma
Learn about Ewing sarcoma
Ewing tumours that start in the bone are known as Ewing or Ewing’s sarcomas. They are the most common type of ‘Ewing tumours’ which also include:
- Extraosseous Ewing tumours (EOE), which start in the soft tissue surrounding the bone. These are also known as ‘extraskeletal Ewing Sarcomas’.
- Peripheral primitive neuroectodermal tumour (PPNET), a rarer Ewing tumour that can occur in the bone or the soft tissue, and shares many features with Ewing sarcoma and EOE.
These tumours are grouped together because they share genetic characteristics or abnormalities.
Ewing sarcoma can develop at any age, but most commonly occur during a person’s early teenage years. In contrast to osteosarcoma which occurs mostly at the ends of our bones, the most common sites of tumour development are in the middle of the hip bones, the rib cage, shoulder blades and the legs.
The genetic mutations that lead to Ewing tumours are fairly well known, with almost all Ewing tumour cells shown to have the EWS gene on chromosome 22 activated all the time. This leads to unnatural overgrowth of the cells. This has happened because of a change or translocation of an important piece of chromosome 22 with surrounding chromosomes, and it can be diagnosed through lab tests. These chromosomal changes are not inherited, and it is still not clear what might cause this mutation to occur.
In some cases, a Ewing sarcoma tumour will show up as a lump or swelling – these are most easily identified on the arms or legs – but the most common symptom is pain.
If there is a lump, it might feel warmer than the rest of the body, and in some cases, symptoms of fever or illness will also present.
With Ewing sarcoma occurring more often in children and teenagers, who experience bumps and soreness from everyday activities, these symptoms will be difficult to identify. However, if the symptoms persist for an unusual amount of time, they should be checked by a doctor.
Additional symptoms will occur if the cancer has spread. For example, if it spreads to the lungs, the patient will probably experience shortness of breath. Or, rarely, when it spreads around the spinal area, a patient might notice weakness or numbness in the arms or legs.
Treatment options between the three Ewing tumour types are comparable, so for the purposes of this information, Ewing sarcoma will be our focus.
Diagnosing Ewing sarcoma
The first action a doctor will probably take is to X-ray the area in which symptoms (lump or pain) are occurring. X-rays often provide sufficient imaging to spot a bone tumour, and also to assess the likelihood that it is an Ewing tumour.
Following this, further imaging scans (MRI scans, CT scans, bone scans and/or PET scans will help to explore the extent or severity of the cancer, and how far it might have spread into surrounding muscle, fat, connective tissue, or other organs.
Ewing sarcoma treatment
If imaging test results strongly suggest Ewing sarcoma, a biopsy will confirm the diagnosis. Bone biopsies are often planned as surgery, due to the difficult locations of the tumour.
In rare cases, if the tumour is contained and in an accessible location, an orthopaedic surgeon might be able to completely remove the cancer. This is called an excisional biopsy. In most cases, however, taking only a piece of the tumour will be possible.
Most often, the patient will be under general anaesthetic, which allows the surgeon to perform other procedures to minimise the need for any follow-up surgery. They might take a bone marrow biopsy, or a biopsy of another location where the cancer is thought to have spread.
During the biopsy, a pathologist can take a quick look at the sample under a microscope. If it looks like a Ewing tumour, the surgeon can place a small flexible tube into a main blood vessel in the chest during the same operation.
This catheter end lies just under or outside the skin and gives doctors easy access to the large vein to administer chemotherapy, while making the treatment less painful for the patient.
Along with chemotherapy, surgery to remove the tumour might be an option. Risks associated with the surgery will depend on the location of the tumour and may include prosthetic bone replacements. These risks and associated rehabilitation after surgery should be discussed carefully with the treatment team.


