Vulval Cancer
Learn about vulval cancer
The vulva is the external part of a woman’s sex organs and consists of soft fatty tissue covered with pubic hair called the Mons Pubis, the labia – consisting of the two outer larger lips (the labia majora), two inner smaller and thinner lips (the labia minora), the clitoris and the perineum (the skin between the vulva and anus).
Cancer of the vulva may involve any of these external female sex organs. The most common areas for it to develop are the inner edges of the labia majora and the labia minora.
Less often, vulval cancer may also involve the clitoris or the Bartholin’s glands (small glands, one on each side of the vagina). It can also affect the perineum.
Types of vulval cancer include:
- Squamous cell carcinoma: Most vulval cancers develop from squamous cells, the skin cells of the vulva. These cancers usually grow very slowly over a few years.
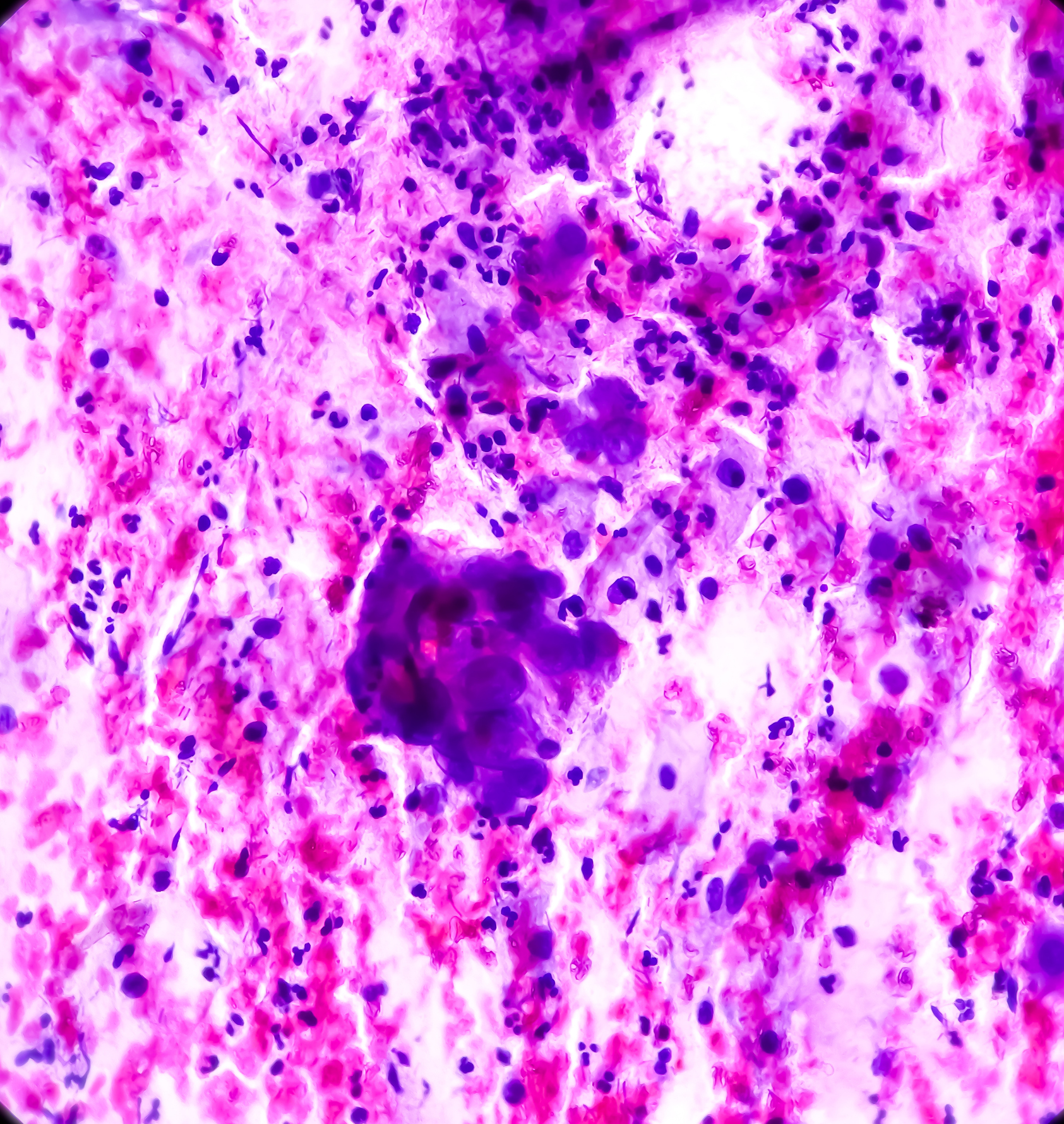
- Vulval melanoma: Vulval melanomas develop from melanin, the cells that produce pigment and give skin its colour. Only about 2 to 4% of vulval cancers are melanomas.
- Adenocarcinoma: These are very rare. They develop from cells that line glands in the vulval skin. Paget’s disease of the vulva is a pre-malignant condition where glandular cells spread outwards and across the vulval skin.
- Verrucous carcinoma: This rare, very slow-growing type of cancer looks like a large wart.
- Vulval sarcomas: These are extremely rare. Sarcomas develop from cells in tissue, such as muscle or fat under the skin, and tend to grow more quickly than other types of cancer.
Vulval cancer symptoms can include:
- A lasting itch
- Pain or soreness
- Thickened, raised, red, white or dark patches on the skin of the vulva
- An open sore or growth visible on the skin
- Burning pain when you pass urine
- Vaginal discharge or bleeding
- A mole on the vulva that changes shape or colour
- A lump or swelling in the vulva
- A lump in the groin
All these symptoms can be caused by other conditions, such as infection but if you have any of these symptoms, you should see your doctor.
The main treatments used for vulval cancer are surgery, radiotherapy and sometimes chemotherapy. A combination of treatments may be suggested depending on the type of cancer, where it is and your general health.
Surgery options include:
- Wide local excision: In this procedure the area containing the cancer is removed along with a border of healthy tissue around it. The important thing is to also remove a border of tissue that is free of cancer cells as this lowers the risk of the cancer coming back.
Sometimes surgeons use a laser to destroy abnormal cells. A laser is a thin, high powered beam of light that your surgeon can use instead of a surgical blade (scalpel).
- Partial vulvectomy: In this procedure you may only need to have just the inner or outer labia removed, or the labia may be removed from one side only. The extent of surgery will depend on where the cancer is, and on how accessible a border of healthy tissue is for the surgeon to work with.
- Vulvectomy (or radical vulvectomy): The whole vulva is removed, including the inner and outer lips of the vagina. The clitoris may be removed as well.
- Lymph node dissection: The lymph nodes on one or both sides of the groin may be removed. The lymph nodes in the groin are usually the first place where cancer cells spread from the vulva. Removing them makes it less likely that the cancer will return. Whether the nodes are taken from one or both sides will depend on the size and position of the cancer.


